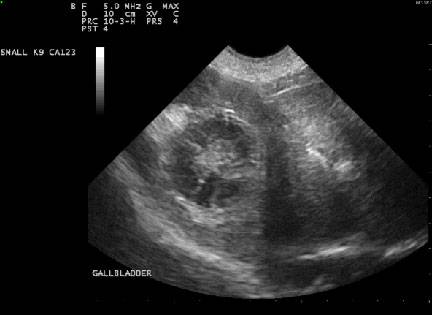
Basic Virology
This virology review is meant to help the beginner understand how viral infections work and how we survive them. Virology is a complicated subject, as is immunology, and the following is meant as a sort of kindergarten of terms and events. We think it is helpful in understanding the biology of what happens with viral infections.
What is a Virus?
Viruses are strange life forms. They have only the bare bones of biochemical equipment, barely enough to even qualify for the title of life form.
- They have only one type of nucleic acid (either DNA or RNA, but not both.)
- They reproduce solely from this nucleic acid, whichever type it is.
- They do not have any metabolic enzymes.
- They are completely dependent on their host cell.
Some Definitions:
Viral Particle
One little individual virus is called a viral particle. Viral particles are so small (some are the size of a large protein molecule) that we cannot really call them creatures; they are more like particles, hence the term. The word virus is more correctly applied to a species or genus of the virus rather than to the individual particles.
Capsid
The nucleic acids (the DNA or RNA) within the viral particles are surrounded by a protein coat and sometimes by an additional fatty envelope. The capsid consists of this protein coat and any fatty layer. The capsid proteins are crucial to the virus’ ability to attach and infect a host cell.
Viruses that have fatty envelopes generally do not last long in the environment as the fat is easily disrupted; these viruses tend to require direct contact with fresh body secretions to transmit the infection.

DNA
DNA is the double-stranded nucleic acid (deoxyribonucleic acid) that serves as the blueprint for all proteins a cell can make. It enables the cell to live and function within a body. It essentially amounts to instructions on how to make different proteins.
Messenger RNA
When it comes time to make a protein, a DNA segment unzips its double strands, allowing messenger RNA to enter and bind. The messenger RNA forms a “negative” image of the DNA segment it is “reading.” The messenger RNA then leaves the cell nucleus and travels out into the cell’s main body, where its message is read by cell structures called ribosomes.
Transfer RNA is another type of RNA that floats around the cell. Each piece of transfer RNA has only three base codes (as opposed to the messenger RNA which has many base codes and is a long strand). The piece of transfer RNA carries with it an amino acid that its code corresponds to.
The ribosome looks like two round pieces attached together. The two pieces grab the strand of messenger RNA and sandwich it between them. The ribosome reads the first three codes on the messenger RNA and matches them to a piece of transfer RNA. It moves to the next three codes and matches them as well. With each match, the transfer RNA leaves its amino acid for the ribosome to bind to the next amino acid, so as the ribosome moves down the strand of messenger RNA, it creates a strand of amino acids based on the matching. As we know, a strand of amino acids forms a protein molecule. This is how our cells make proteins.
Transcription
The act of messenger RNA taking down the protein code from the original DNA segment is called transcription.
Translation
The act of producing a protein from the segment of messenger RNA using transfer RNA is called translation. It is performed by the ribosomes mentioned previously.
Viral Infections
When the match is correct, the virus binds to the cell and injects its nucleic acids inside. There are several techniques that viruses use to accomplish this, but all involve the capsid. Once the viral particle has injected its nucleic acids into the host cell, the next activity is to manufacture messenger RNA for the cell to translate into protein. The proteins that the viral nucleic acids make will shut down the cell’s normal function and convert the cell into a factory for viral particle production.
- Some viruses simply contain ready-made messenger RNA and they just inject it into the host cell (like polio).
- Some viruses inject a negative of the messenger RNA they need and include with it an enzyme that will trick the host into making the usable messenger RNA from the negative (like rabies).
- Some viruses inject their DNA directly into the host cell. Messenger RNA is made from this DNA, just as it would be made from host DNA (like poxviruses).
Regardless of the tricks the virus uses to make messenger RNA, once the messenger RNA is made, the host cell is doomed. Ribosomes line up on the strand of messenger RNA, read it, and use transfer RNA to mass produce the protein coded. This will be a viral protein, and its action will be to shut down normal cell function and dedicate the cell to the production of viral capsid and viral DNA.
Soon the host cell is little more than a bag of viruses. These viral particles either bud off the surface of the host cell or the host cell simply explodes, leaving millions of new viral particles to seek new host cells. The only way to stop this process is for the immune system to recognize the infected cell early and destroy it before virus production becomes too advanced.
Infected cells express viral proteins, shapes that the immune system can recognize. Within the body are several groups of cells, all created to respond against a specific shape. For example, B lymphocytes, which live in our lymph nodes, transform into antibody-producing plasma cells once they encounter their destined antigen. They produce Y-shaped antibodies that flood the circulation and bind the viral antigen, thus preventing the virus from attaching to the host cell, clumping with other antibody-virus groupings to create a larger clump, which in turn attracts a cell called a macrophage. The macrophage is the body’s “Pac Man,” swallowing and digesting debris.
Aside from antibodies, there are patrolling T-lymphocytes that identify viral or other inappropriate shapes on the surfaces of host cells. The T-cell can thus recognize a virally infected cell or even a cancer cell, attach, and destroy it before it causes harm.
Hopefully, between T-cell and antibody attack, the viral infection is removed from the body, and the status quo resumes.