Canine Heartworms and Preventing Disease
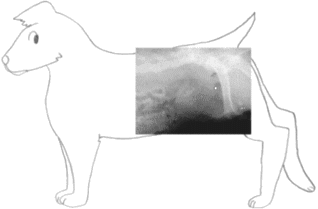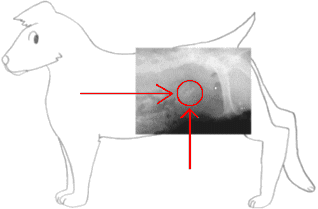
Canine heartworms, Dirofilaria immitis, are parasitic worms that pose a serious threat to dogs. These long, slender worms live in the pulmonary arteries (and, occasionally, within the heart) of dogs and can measure up to a foot in length. They can cause substantial damage to the lungs and heart.
Adult heartworms cause inflammation of the blood vessels in the lungs, resulting in respiratory issues and pulmonary hypertension. In some cases, this leads to weight loss, weakness, right-sided congestive heart failure, reduced quality of life, and even death.
The prevention of heartworms and early detection are crucial in managing heartworm disease.
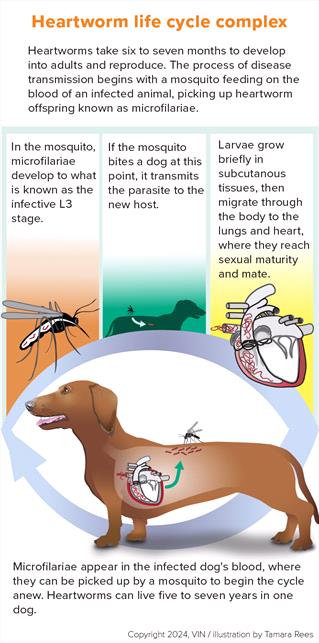
Mosquitoes and the Heartworm Lifecycle
Mosquitos are vectors of heartworm disease. A vector is a carrier and transmitter of disease from an infected individual to a non-infected individual. Certain species of mosquito can ingest young heartworms, called microfilariae when they feed on an infected animal. Once inside the mosquito, the microfilariae develop into third-stage larvae (known as L3) over a few weeks, provided that the environmental conditions are conducive (temperatures above 58oF). The larvae pass through the puncture wound the mosquito makes when it bites another animal.
The larvae grow under the skin of the newly infected animal over several weeks, progressing through additional larval stages. At a certain point, the larvae enter the bloodstream and float into the pulmonary arteries (the arteries carrying blood from the heart to the lungs). Here, they mature into adults. It takes about six to seven months for the larvae to reach adulthood. Adult heartworms mate, and then the females begin to release tiny larvae, the microfilariae, back into the bloodstream, continuing their lifecycle.
Prevention is Key
Preventing heartworms is much easier (especially for your dog) than having to treat an active heartworm infection.
Studies show that exposure to heartworm depends on factors such as:
- The presence of wild canine populations (foxes, coyotes, wolves) in the surrounding area can continue the spread of heartworm.
- Regional differences in climate and ecosystems (elevation, humidity, rainfall, temperature)
The Prevalence of Heartworms Around the World
Heartworms exist in many parts of the world, but the prevalence greatly varies. In warmer climates with higher mosquito populations, such as tropical and subtropical areas, the risk of heartworm transmission is higher. These areas make excellent habitats for mosquitoes and the development of heartworm larvae, so dogs living in these regions are at a greater risk of heartworms. On the other hand, there are fewer heartworm infections in cooler or drier regions with smaller mosquito populations.
The travel, relocation, and presence of infected animals can allow heartworms to start infecting animals where they are less common. Climate change (and temperature increase) is also expanding mosquito ranges, creating longer active seasons and better environmental conditions for larvae.
Environmental Considerations
More recent recommendations for preventing heartworm infections advise reducing mosquito bites. This can be done by avoiding places with heavy mosquito populations when possible to reduce the chances of being bitten and contracting heartworms (for example, some studies have shown that indoor dogs in high-risk areas tend to have fewer infections than outdoor dogs).

Avoid visiting permanent and semi-permanent (seasonal) bodies of water like lakes, streams, and floodplain areas with your dog, especially when large mosquito hatches are taking place (usually in warmer, humid weather). Check around your home for areas with standing water and eliminate containers or reservoirs that may be prime real estate for mosquito larvae.
There may always be an ideal climate for mosquitoes, and other preventative methods such as lawn alteration, porch nets, and other mosquito barriers may be helpful, depending on your location. Talk to your local health department if you have concerns about mosquitoes on your property and what you can do to help control them.
Preventative Medications
Heartworm preventatives are prescribed by your veterinarian and come in oral, topical, and injectable forms. As mentioned before, preventing heartworms is much easier than treating them, and the American Heartworm Society recommends FDA-approved heartworm preventatives year-round.
In areas where mosquitoes are endemic (native or regularly present), your dog can be infected if just one preventative dose is missed. The risk varies depending on your location, and even people who live in places with cold winters should give heartworm preventatives year-round for the best possible prevention.
Detecting Heartworm Infection
Blood tests for heartworm infections are recommended yearly for all dogs over seven months. If you do not give preventatives regularly every month or if you switch preventatives, more frequent testing may be recommended. If your dog has tested positive for heartworms, your veterinarian will discuss the treatment options available.