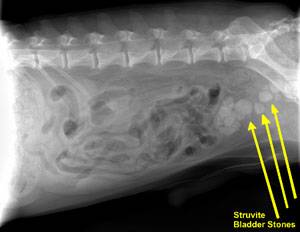
There are many types of bladder stones, and each tends to form in a specific breed or species under specific conditions.
Oxalate Bladder Stones in Dogs
- 73% of calcium oxalate patients are male.
- Breeds at especially high risk include miniature schnauzers, Lhasa Apsos, Yorkshire terriers, miniature poodles, Shih Tzus, and Bichon Frises.
- Most cases occur in dogs between ages 5 and 12 years of age.
How Are Stone Types Determined?
Although a urinalysis can provide a clue, the only way to know for sure that a dog’s bladder stone is an oxalate is to retrieve a stone and have a laboratory analyze it. If the stones are very small, flushing the urinary bladder and expressing it (known as voiding urohydropropulsion) may not only produce a stone sample for testing but remove all the stones and alleviate the current signs. When stones are too large to fit out the urethra, they can be removed to resolve signs and obtain sample stones by surgical removal from the bladder (the traditional method), retrieving them by sending a cystoscope up the urethra, or by using laparoscopy (percutaneous cystolithotomy – PCCL) to send a cystoscope through a small incision into the abdomen and then into the bladder and using a grabbing device in the cystoscope channel to retrieve them. Calcium oxalate stones cannot be made to dissolve over time by changing to a special diet (as can be done with struvite or uric acid bladder stones).
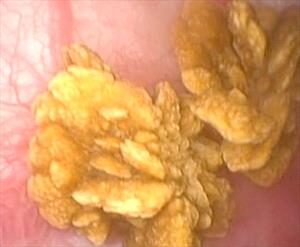
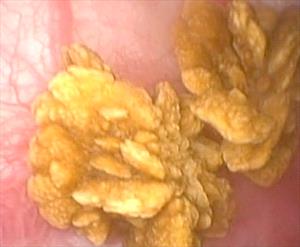
This endoscopic photograph of calcium oxalate bladder stones are in a dog. Bladder stones can be detected during periods of urinary discomfort or they might be discovered incidentally as a surprise. If allowed to remain in the bladder, they can lead to on-going infection, urinary obstruction or continuing discomfort so they must be addressed. Preventive measures must be taken to avoid the formation of new stones. Photo by Dr. Craig Stanton.
Why Would My Dog Form Calcium Oxalate Stones?
It shouldn’t be too surprising that there is a strong hereditary component to forming oxalate bladder stones; this is also true in humans. There is a substance (called nephrocalcin) in urine that naturally inhibits the formation of calcium oxalate stones.
This substance can be defective in both humans and dogs who form calcium oxalate bladder stones. This has been demonstrated in Miniature Schnauzers. Other breeds, such as English Bulldogs and related breeds have Hereditary Calcium Oxalate Urolithiasis Type 1, which is noteworthy for earlier age at the initial development of stones. There is also a Type 2 disorder from a different mutation. There are other potential genetic causes as well.
There is a bacteria that exists as part of the normal flora of the GI tract that metabolizes oxalate. Antimicrobial use may eliminate this good bacterium altogether. This would be expected to increase calcium oxalate stone risk and is being studied.
In humans, the genetic predisposition for stone formation is coupled with dietary issues (problem foods include spinach, peanuts, chocolate, dairy products, calcium supplements, vitamin C supplements, and tea). Dogs are more likely to eat simply a commercial brand of dog food without nearly the dietary variety that humans experience. This means that diet can often be used to manage the problem in the dog unless genetics (not diet) is the cause.
There are some metabolic diseases that might predispose a dog to create a calcium oxalate stone. For example, a dog with Cushing’s disease will be overproducing cortisol (commonly known as cortisone). This hormone increases calcium excretion in urine. The extra calcium present in the urine will promote a stone. Some animals may have an elevated blood calcium level (hypercalcemia) for any number of reasons, and this could lead to excess calcium in the urine as the body attempts to restore calcium balance. Again, extra calcium in the urine promotes a stone. Screening for such medical conditions is important and is generally part of the medical workup once stones are detected on a radiograph. If any such metabolic problems are uncovered, they will need to be treated separately. As these problems are resolved, no further stone prevention measures should be needed. Because of the complexity involving a variety of different causes and risk factors, this should be viewed as a group of diseases that result in the same endpoint, calcium oxalate stones. The specific cause does change what prevention measures are expected to help. Clues based on the breed can help; but it can be very difficult to know which disease and risk factors are present in any given dog, contributing to the high recurrence rate of these stones in dogs.
Why Can’t The Stones Stay Where They Are?
The most immediate concern for the dog with bladder stones is that the urinary opening may obstruct as the dog attempts to pass the stones. This is largely a male dog problem but the results can be life-threatening uremic poisoning. In such cases, the veterinarian will try to dislodge the stone, flushing it back into the bladder to restore the patency of the urinary opening. If the stone cannot be dislodged, a new urinary opening may have to be surgically created. The urethra (the narrow tube connecting the urinary bladder to the outside world) is a difficult place to perform surgery, so it is preferable to move the stone back into the bladder for removal rather than attempting removal from the urethra.
Bladder stones are irritating to the bladder simply by rubbing on the tender bladder lining. Bleeding typically results, and, of course, the chance of developing chronic bladder infections is markedly increased with the presence of bladder stones.
Because calcium oxalate stones cannot be dissolved by diet change, removing the stones is usually necessary. Studies have shown that 50% of dogs who have undergone such surgery will develop new calcium oxalate stones within three years unless proper prevention is instituted.
The following therapeutic plan has been devised to minimize the chance of recurrence after the stones have been removed.
Step One: Diet
While special diets cannot dissolve existing stones, they do help prevent new stones from developing. Prevention centers on creating a urinary environment with minimal calcium and oxalate as well as creating a urine pH that is not conducive to calcium oxalate formation.
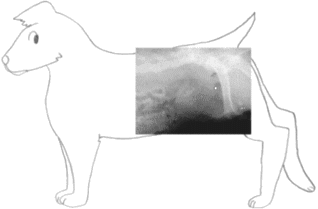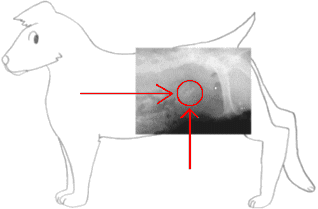
Illustration by Wendy Brooks, DVM
Further, high protein, high sodium diets should not be used and diets low in phosphorus may stimulate vitamin D production and could increase calcium absorption. Commercial specialty foods with these requirements are available. Work with your veterinarian to find an appropriate diet.
For each of the commercially available diets, the canned form is preferable to dry to increase water consumption and thus help dilute the urine. It is especially important to avoid table scraps when caring for an oxalate stone-forming dog. Still, no one wants their dog to live life without treats.
The following treats are acceptable for oxalate stone-forming dogs:
- Plain, cooked chicken
- Plain, cooked turkey
- eggs
- rice
- peas
- pasta
- white potatoes
- cabbage
- cauliflower
- bananas
- melon
Selecting a diet that actually prevents stones but is also desirable to the picky pet may be challenging. It may be possible to have a veterinary nutritionist provide a recipe for an appropriate home-cooked diet. Please visit www.balanceit.com or www.petdiets.com for details.
Some medications can increase the risk of calcium oxalate stone development, and these should be avoided. Prednisone and other cortisone-type medications (commonly used for itchy skin, arthritis, inflammatory bowel disease, and other inflammatory conditions) should be avoided if possible. Furosemide (brand name: Lasix or Salix) is a diuretic mostly used in the treatment of heart failure. Both these medications lead to excess calcium in the urine. Should a diuretic be needed for a patient at risk for calcium oxalate stones, one from the thiazide class (see later) would be a better choice. Supplementation with Vitamins D or C also increases the risk of forming oxalate stones; such supplementation should be discontinued.
Step Two: Urinalysis and Radiographs
Two to four weeks after surgery, a urine sample is checked and the bladder is radiographed. If the urine is not adequately diluted (meaning the specific gravity is less than 1.020), water consumption will have to be increased (either by adding water to the food or increasing the amount of canned food).
If urinary pH is less than 6.5 or if oxalate crystals are seen, it is time to go to Step Three. If all is well, a urinalysis should be performed every three to six months or so for the rest of the dog’s life (the University of Minnesota’s current recommendation).
Radiographs are also taken every 6-12 months so that any new stones will still be small enough to be retrieved from the bladder by flushing. If you skip this monitoring, you may find stones have developed to a large size, and surgery is again needed to remove them.
Step Three: Potassium Citrate
By taking potassium citrate pills, citrate levels increase in the urine. Calcium binds to the citrate instead of the oxalate. This is a desirable event since calcium citrate tends to stay dissolved, whereas calcium oxalate tends to precipitate out as a mineral deposit. Potassium citrate also helps create alkaline urine (in which calcium oxalate stones have difficulty forming). Potassium citrate supplements are typically given twice a day.
Step Four: Urinalysis Again
Two to four weeks after potassium citrate is added to the therapeutic diet, a urine sample is checked. If the urine is not adequately diluted, water consumption will have to be increased either by adding water to the food or increasing the amount of canned food.
If urinary pH is less than 6.5 or if oxalate crystals are seen, it is time to go to Step Five. If all is well, urinalysis and radiographs should be performed every 6-12 months or so for the rest of the dog’s life (the University of Minnesota’s current recommendation). In other words, if the urinalysis shows all the desired parameters and radiographs show no new stones forming, then therapy is working, and the pet can go on a regular monitoring schedule. If testing shows the patient is still predisposed to stone formation, it is necessary to proceed down this list until control is achieved. Again, radiographs should be taken every six to 12 months.
Step Five: Thiazide Diuretics
A diuretic is a medication designed to increase the amount of urine produced. The thiazide class of diuretics does this in a way that reduces the calcium content of the urine. This medication is typically given twice a day and electrolytes are generally measured via blood test within the first two weeks of this treatment.
There will always be some dogs who continue to form stones no matter what is done. With radiographic monitoring, it is hoped that new stones can be detected while they are still small. As research continues, new developments may arise that will not require such frequent monitoring.
A Note On The Bichon Frise
The Bichon Frise appears to have a unique situation with oxalate bladder stones in that they seem to begin to recur virtually as soon as they have been removed. In a study presented by Jody Lulich’s group at the University of Minnesota at the 2004 meeting of the American College of Veterinary Internal Medicine, 24 out of 33 Bichons had oxalate stone recurrence after cystotomy (37% had had their first recurrence in the first year after surgery, by the end of the second year 57% had recurred, and by the end of the third year 73% had recurred, some more than once). Steps to prevent recurrence need to be particularly aggressive from the beginning in this breed as they seem to have 20 times the risk of oxalate stone formation compared to other breeds.
Preventing Male Dog Obstruction
In male dogs, a bone called the os penis is located in the penis, surrounding the urethra. Urine passes through this hollow bone like water through a pipe. Because this area is made of bone, it cannot stretch or expand to accommodate a stone trying to pass. A stone blockage of this type leads to an emergency and death if it goes untreated.
In a perfect world, controlling the bladder stones controls the risk of obstructions, but controlling the bladder stones is not always easy, and treating a dog over and over for obstruction becomes expensive. A surgical procedure called a urethrostomy can be performed to prevent obstruction. This procedure involves creating a new urinary opening in the area of the scrotum. This allows urine to be expelled earlier in its course so that passage through the os penis does not occur. The flexibility of the non-bony part of the urethra plus the surgically enlarged urinary opening allows for smaller stones to pass rather than stick in the os penis.
To perform this surgery, the male dog must be neutered (which can be done at the time of the urethrostomy). The creation of the new opening usually requires the removal of the empty scrotum.
While this is not as good an outcome as preventing stone recurrence, at least the emergency obstruction is prevented.
Calcium oxalate bladder stones can be frustrating. Not only do they tend to recur, but following monitoring recommendations involves a visit to the veterinarian’s office every three to six months. It is up to every owner how rigid to be with guidelines, but keep in mind that the trouble and expense of a stone surgery weigh against the much less trouble and expense of monitoring.
Laser Lithotripsy
A new technique of stone removal involves the use of a laser to blast the stone into pieces small enough to pass. This option (called laser lithotripsy) is especially useful when the number of stones present is small and/or when a stone is lodged in the urethra and cannot be flushed into the bladder. It will not be helpful for a large number of stones as the process would be too time-consuming relative to a more conventional approach but for the right patient, it is less invasive than other procedures.