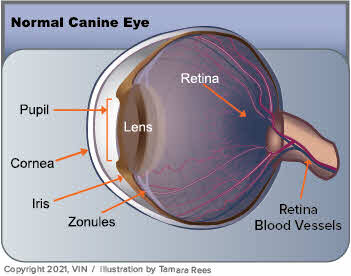
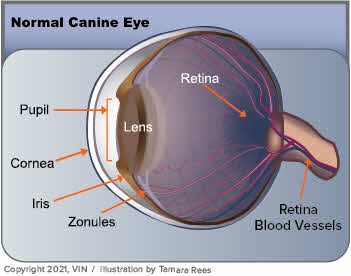
What Is Clostridium difficile?
- Clostridium difficile is a species of bacteria that can be found in the intestinal tract of humans and many animal species, including pets, farm animals, and wildlife.
- Clostridium difficile is an important cause of disease in people and animals.
- These bacteria do two very important things:
Some strains contain genes that allow them to produce toxins. It is the toxins, not the bacteria themselves, that make a person or an animal sick.
They can form spores, which can survive for years in the environment and are resistant to many disinfectants. If ingested, the spores germinate and the bacteria begin to grow when they reach the intestine.
- In people, C. difficile is most common in the elderly, hospital inpatients, and individuals on antibiotic therapy. It usually causes diarrhea, which may be mild or very severe.
- The strains of C. difficile that infect pets are often the same as those that infect people, but it remains unclear if animals can transmit C. difficile to humans.
How Common Is Clostridium difficile?
Humans
In developed countries, C. difficile is the leading cause of infectious hospital-associated diarrhea in adults and accounts for 15-25% of cases of antibiotic-associated diarrhea. It is becoming more common in North America.
The most important risk factor for C. difficile infection (CDI) is treatment with antibiotics. The antibiotics affect the normal “good” bacteria in the intestine, which sometimes allows C. difficile to take over and grow faster.
Old age, certain cancer treatments, long hospitalization, some acid-suppressants used to treat stomach ulcers, intestinal surgery, and some other procedures also increase the likelihood of CDI.
A hyper-virulent C. difficile strain (ribotype 027/NAP1) has emerged in North America, Europe, and Japan, and has been responsible for epidemics of severe illness in hospitalized patients.
Recently, severe illness due to CDI has been reported in some healthy, non-hospitalized people as well.
Animals
A small percentage of healthy dogs and cats (0-4%) carry C. difficile in their intestine. But in puppies, kittens, animals in breeding colonies, and dogs that visit human hospitals, the percentage may be higher (up to 30%). The bacteria can also be found in other types of pets, but it is unknown how common this is.
- Usually, C. difficile never causes any illness in these animals.
- As in people, treatment with antibiotics increases the likelihood that a dog may be shedding C. difficile in its stool. Contact with children may also be a risk factor for C. difficile shedding in dogs.
How Do Animals And People Become Infected With C. difficile?
Clostridium difficile lives in the intestine of people and animals. When the bacteria are passed into the stool, they form spores that can survive in the environment for a long time.
The bacteria are transmitted when the spores are ingested. This typically happens when there is stool contamination on something a person touches, and then the person touches their nose or mouth. Contamination of food and water can also be a problem.
It is unclear if C. difficile can be transmitted from pets to people. The types of C. difficile found in pets are often the same as those found in people, including the epidemic strain ribotype 027/NAP1. So it makes sense that C. difficile could potentially be transmitted between people and animals, but there is still no conclusive proof.
For now, it is best to err on the side of caution and consider C. difficile transmissible between pets and people until proven otherwise.
What Happens If A Person Or Animal Gets Clostridium difficile Infection (CDI)?
Humans
In people, CDI (which is also sometimes called C. difficile-associated disease, or CDAD) may cause no illness at all, or anywhere from very mild to very severe diarrhea. Additional complications can also occur, particularly in people who are already sick for another reason. In some cases, the disease can be fatal.
Animals
The vast majority of dogs and cats that carry C. difficile in their intestine do not become ill. However, there does appear to be a link between C. difficile and diarrhea in dogs in some cases, and there is one report of C. difficile possibly causing diarrhea in two cats. In most of these cases the diarrhea is mild, and clinically appears the same as diarrhea due to other common causes. Occasionally, more severe illness and diarrhea may occur.
How Is Clostridium difficile Infection Diagnosed?
In animals and people, CDI is diagnosed by testing the stool for the toxins that are produced by the bacteria. Just finding C. difficile (by culturing the stool, for example) does not mean that it is causing a problem because not all strains can produce toxins. Even strains that can produce toxins don’t produce them all the time, so the bacteria can be found in perfectly healthy people and animals. Detecting the toxins themselves is the key. Testing animals that do not have diarrhea for C. difficile is not recommended.
How Is Clostridium difficile Infection Treated?
In humans, many cases of CDI are caused by treatment with antibiotics for some other infection. In mild cases, diarrhea may resolve with no additional specific treatment. In severe cases, other antibiotics may be needed to control C. difficile. Probiotics are not considered effective for the treatment of CDI in humans.
Some (if not most) cases of CDI in pets resolve without additional antibiotics. If the animal has a lot of diarrhea it may need to be given fluids to prevent dehydration.
There is no vaccine available for C. difficile for any species.
If you (or your pet) develop diarrhea while being treated with antibiotics, tell your physician or veterinarian right away. However, it is very important you only stop or change the medication you are taking or giving to your pet if you are told to do so by your physician or veterinarian. Otherwise, the infection for which the antibiotics were originally prescribed may get worse.
What Do I Do If My Pet Is Diagnosed With Clostridium difficile?
- Wash Your Hands!!!: Wash your hands with soap and running water after handling your pet, and especially before handling food or touching things in the kitchen.
– Alcohol-based hand sanitizers are unlikely to kill C. difficile spores, so ideally you should wash with soap and water instead.
- Follow Instructions: It is important to follow all treatment instructions given by your veterinarian, particularly regarding any prescription medications. If you have questions or are having trouble with the treatment, call your veterinary clinic to let them know.
- Steer Clear of Stool: Avoid contact with your pet’s stool as much as possible. Wash your hands thoroughly after handling any stool, even if you use a plastic bag or a scoop to pick it up.
- Clean Up Quick: If your pet accidentally passes diarrhea in the house, clean it up as soon as possible. Wearing rubber gloves, remove as much of the stool and fluid as possible using disposable towels that can be placed in the garbage right away. Then disinfect the area with dilute household bleach (1 part bleach to 10 parts water), if it is a surface such as tile that won’t be damaged. Thoroughly wash your hands after cleaning.
For surfaces that can’t be bleached, thorough cleaning is the most important step to physically remove as much contamination as possible. Steam cleaning is a reasonable way to reduce the number of C. difficile spores that may be left in rugs, carpets, or similar floor coverings.
- Other Pets: It is not known how much of a risk one infected pet is to other pets. It is prudent to keep pets diagnosed with C. difficile away from other pets (e.g. avoid parks and boarding facilities) until their diarrhea has resolved.
Therapy Animals
Visiting healthcare facilities is a risk factor for C. difficile shedding in dogs. However, it is unclear whether therapy pets that visit hospitals and nursing homes have an increased risk of developing C. difficile diarrhea. Healthy animals do NOT need to be tested or treated for C. difficile. There are guidelines available to help reduce the risk of pets acquiring infectious diseases in hospitals, which should be followed if your pet is part of a visitation program. These include
- Not letting your dog drink out of the toilet when in a hospital or nursing home.
- Not letting patients feed your pet treats. This can increase the likelihood that a dog will shed C. difficile, probably because dogs lick C. difficile off the hands of the patients.
If I Have Clostridium difficile, Should I Test My Pet?
NO. Even if your pet was found to be shedding C. difficile in its stool, you still would not know if it was the same strain you were carrying. This type of specialized testing is not readily available and is not indicated in most situations.
If you have C. difficile, you should be very thorough about washing your hands after using the washroom. Also try to prevent your pet from drinking from the toilet, if it tends to do so.
The risk of disease to the general population posed by C. difficile in house pets such as dogs and cats is:
Healthy Adults
Individuals with compromised immune systems (e.g. HIV/AIDS, transplant, and cancer patients) are more susceptible to many kinds of infections, including those which may be transmitted by pets. While these individuals are not advised to get rid of their pets, precautions should be taken to reduce the frequency of contacts that could result in pathogen transmission (e.g. avoiding contact with any animal feces), as well as the ability of infectious agents to survive in the household (e.g. prompt and thorough disinfection of potentially contaminated surfaces).
Infants and young children (less than 5 years old) are more likely than adults to extensively handle animals if given the opportunity, more likely to touch their faces or mouths, and less likely to wash their hands after handling an animal. Children may “snuggle” with pets such as dogs and cats; this very close contact can increase the risk of disease transmission.
Young children should be supervised when playing with animals, and an adult should ensure that they wash their hands afterward, especially before handling food. Older children should be taught to do the same.
It is important to note that infants less than 12 months of age are not affected by C. difficile.
For these groups, the zoonotic risk posed by C. difficile in house pets such as dogs and cats is likely: