Canine distemper virus, also referred to as CDV, canine morbillivirus, and hardpad disease, is a highly contagious disease affecting not just dogs but many animals. Distemper occurs worldwide, and dogs are the primary carriers of the disease.
Canine distemper virus can sometimes occur along with other respiratory infections, including bacterial diseases such as Bordetella bronchiseptica, and Streptococcus equi sub. zooepidemicus, fungal diseases like Mycoplasma spp., and viruses, including canine influenza virus, respiratory coronavirus, parainfluenza virus, adenovirus, and herpesvirus.
CDV is commonly spread through droplets or spray from the nose and mouth, such as through sneezing or coughing. However, infected dogs can shed the virus in nearly all bodily fluids. CDV is carried to local lymph nodes within 24 hours of contact with cells in the airways and lungs. Within a few days, the virus spreads to the spleen and abdominal lymph nodes, then spreads through the blood to cells of the gastrointestinal (GI) tract, urogenital tract, and central nervous system (CNS). The CNS tissues are typically infected by day eight or nine when neurological signs can be seen.
When the body’s immune system is triggered by exposure to disease, it reacts by producing antibodies. These antibodies are made up of proteins that attack the virus or bacteria causing the infection, hopefully protecting the body from getting sick. How strong your dog’s immune system is will play a big part in how sick they become after exposure.
If an animal’s immune system can be activated to begin making antibodies to fight CVD by the 14th day after exposure, the signs of the illness may not be noticed.
Dogs with mild to intermediate immune responses and delayed antibody titers (this means your dog may test negative on distemper tests but still have the infection) will develop clinical signs. While the virus can eventually be cleared as antibody levels rise, it may persist for extended periods in the eye, the central nervous system (including the brain, brainstem, and spinal cord), and some skin tissues (e.g., footpads).
By days nine to 14, dogs without good immune responses tend to experience severe clinical signs and can die suddenly.
Diagnosis
Diagnostic testing starts with a physical exam and includes bloodwork, antibody tests, cytology/histopathology of affected tissues, X-rays, cerebral spinal fluid analysis, eye exams, and PCR testing. Sometimes, unfortunately, a CDV diagnosis can’t be made prior to death, and a final diagnosis can be determined only after a veterinary pathologist has examined the body.
Animals Affected By Distemper
- cat
- jackal
- coyote
- hyena
- lion
- tiger
- leopard
- ferret
- fox
- weasel
- raccoon
- seal
- sea lion
- dolphin
- Giant panda
- certain primates
Health History and Signs
Dogs with mild distemper cases may exhibit a lack of energy, decreased appetite, fever, coughing, shortness of breath, and nasal discharge.
Dogs with more severe clinical disease may show fever, nasal discharge, conjunctivitis, coughing, difficulty breathing, vomiting, diarrhea, weight loss, and dehydration. Secondary bacterial infections can occur and can make the signs worse.
Your dog may also experience signs that the central nervous system is involved, such as ataxia (incoordination), limb weakness, myoclonus (involuntary rhythmic muscle twitching), stiff neck, and hyperesthesia (skin sensitivity). These signs can occur at the same time or up to three weeks after the onset of CVD and typically get worse over time. Older dogs that have some immunity are more likely to have no signs or just mild disease.
Eye problems include keratoconjunctivitis sicca (dry eye), anterior uveitis (inflammation of the front part of the eye), and damage to the retina (which allows the brain to process sight). The optic nerves, which carry information to the brain from each eye, may develop optic neuritis (swelling and inflammation), leading to blindness.
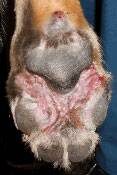
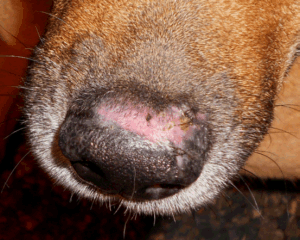
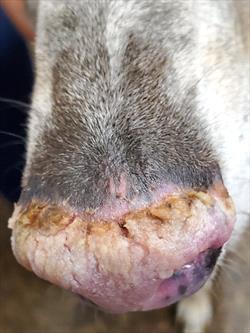
Skin problems in puppies include pustular dermatitis (blister-like sores that can be chronic), and the skin of the nose or toe pad can develop hyperkeratosis (skin thickening). When this happens in the toe pads, it is referred to as hardpad.
Infections in puppies can cause enamel hypoplasia (damage to the developing teeth). Cardiomyopathy, or enlargement of the heart muscles, which may lead to cardiac issues, is possible. Growing puppies have developed hypertrophic osteodystrophy, (when bones in the legs grow abnormally), causing pain.
Abortion and stillbirths can occur in pregnant dogs.
Ulcers of the mouth can occur, but they tend to be rare.
Clinical signs will vary, depending on which strain of the distemper virus is involved and how well your dog’s immune system responds to the infection. Older dogs that have some immunities are more likely to have no signs or just mild disease. Puppies and animals with no immunity are more likely to have severe clinical signs.
Treatment And Management
Currently, no specific treatments are available for CDV.
Supportive care can include fluid therapy, antibiotics for secondary bacterial infections, lung treatments for bronchopneumonia, anti-nausea and vomiting medications, steroids, anti-seizure medications, etc. Supportive care will vary, depending on which parts of your dog’s body have been affected.
Prognosis
The prognosis depends on the viral strain and your dog’s immune response. Older dogs with a good immune response may not have symptoms or a mild disease. Puppies or those with a poor immune response tend to develop more severe disease.
The most important factors affecting your dog’s prognosis are neurologic. The prognosis for dogs that have neurological problems (the brain, spinal cord, and other nerves are affected) is guarded to poor, and there is a 50% chance of death. Dogs that recover may be immune to reinfection for long periods and may be immune for life.
Prevention
Hospitalized dogs with CVD must be isolated from other dogs. Dogs usually shed the virus in urine, stool, saliva, nasal mucous, etc., for one to two weeks after the initial infection. Dogs with neurologic signs can shed the virus for longer periods of time. Extended quarantine may be necessary to prevent the spread to uninfected animals.
CDV is susceptible to many disinfectants. Talk with your veterinarian about how to best disinfect areas, dishes, and toys when your dog comes home. Good hygiene practices (e.g., handwashing, wearing gloves/protective clothing) are recommended when handling infected dogs.
Vaccination
Vaccination is crucial in preventing your dog from getting CDV. Current guidelines recommend vaccinating dogs at six to eight weeks of age and repeating the vaccine every three to four weeks until the puppy is 14 to 16 weeks of age. Dogs would then receive another vaccine one year after the initial series and then every three years afterward.
Distemper antibodies that puppies could have received from their mother’s milk (colostrum) in the first few feedings, and that could prevent the vaccinations from working, are typically gone by 12-14 weeks of age. In dogs that are more than 16 weeks old, the initial vaccination series can consist of two vaccines given two to four weeks apart.
The majority of dogs develop protective antibody levels within one to two weeks following vaccination.
Zoonotic Potential
A zoonotic is a disease that can be transferred from animals to humans. There is some concern that humans might be susceptible to the canine distemper virus because of recent CDV infections in primates. Because CDV is similar to the human measles virus, additional concern has been raised because of the decrease in routine measles vaccination by many humans. However, at the time of this writing, no evidence exists that CDV can infect humans.