Nebulizer Use for Dogs and Cats
Dogs, cats, and other pets who develop lung diseases such as pneumonia, asthma, kennel cough, bronchitis, and so on can benefit from a nebulizer delivering saline, albuterol, antibiotics, or other drugs. A nebulizer is a machine that aerosolizes medicine into a fine mist; it’s like spraying medicine. A face mask is held over the pet’s muzzle (most pets can learn to accept the face mask) so that medication is inhaled deep into the respiratory tract.
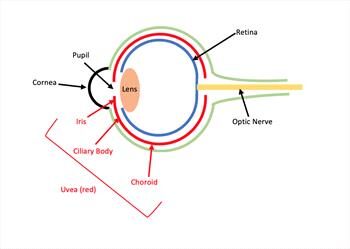
The esophagus lies above the trachea and is protected by the epiglottis. Pneumonia may result from infections caused by kennel cough, viruses and bacteria. Pets with megaesophagus are prone to developing aspiration pneumonia because they tend to regurgitate food and fluids into the back of the throat and then aspirate the material into the lungs.
A nebulizer can be purchased from human medical supply stores, online, or from eBay. There are several good nebulizer brands, such as Pulmo-Aide, Omron, Devilbiss, etc. Make sure that you obtain the compressor (the machine), tubing, and the medication cup. The tubing, T-piece (a t-shaped tube that attaches the machine to the pet and to an exit) and medicine cup are called a nebulizer kit.

A vaporizer is not the same as a nebulizer. A vaporizer is typically used for sinus or upper respiratory issues rather than lung issues. Vaporized droplets are too big to get as deeply into the lungs the way nebulized particles
You can purchase an appropriately sized mask from a veterinarian, or make one yourself.
Using a Nebulizer
Follow these steps to use a nebulizer.
- Plug in the compressor.
- Insert one end of the tubing into the compressor and the other end into the cup.
- Place the correct dose of the medicine in the medicine cup.
- Start the compressor.
a. Keep the cup up straight and hold the mask up to your pet’s face. You might want to practice placing the mask against the pet’s face before using the nebulizer

- b. Put a little canned dog/cat food, baby food, cream cheese or peanut butter inside of the mask and allow the pet to lick it. This can also distract a pet while the treatment is proceeding.
- After 5 to 10 minutes, you’ll see and hear that the medicine is running out.
- Shake the cup downward a few times to make sure all the medicine has come through.
- Take apart the plastic parts of the nebulizer and wash all the parts.
Cleaning the Nebulizer
Bacteria and viruses can live and reproduce in a nebulizer that is not routinely cleaned.
After each use, swish each piece in warm running water. At the end of the day, after you use it the last time, scrub each piece with warm soapy water. Rinse each piece under warm running water. Let each piece air-dry on a clean dish towel or paper towel. When the pieces are completely dry, put the nebulizer back together. If not using for a period of time, store it in a clean, dry bag.
Twice each week, or after the treatment is completed, mix a half cup of white vinegar with 1.5 cups of tap water. Soak each piece in this mixture for one hour. Rinse each piece under warm running water. Let each piece air-dry on a clean dish towel or a paper towel. When the pieces are completely dry, reassemble the nebulizer.
What do I do if I have Cleaned my Nebulizer and the Tubing is still Wet?
The easy way to dry the tubing is to attach it to the compressor. Then switch on the machine, and let it run for a minute or two. The blowing air will dry out the tubing. Use a paper towel or clean hand towel to dry the other parts.
What Medications can be Given with a Nebulizer?
A variety of drugs can be given using a nebulizer: bronchodilators like albuterol (open up the bronchioles allowing debris to more easily be removed from the lungs), steroids, water-soluble antibiotics, saline, N-acetylcysteine, etc. Albuterol opens up the bronchioles, making it easier to breath and allowing antibiotics to get deeper within the lungs. As albuterol can increase the heart rate, it should be used with caution in dogs with heart disease. Do not exceed three treatments per day unless advised by your veterinarian. The dose of albuterol may need to be adjusted based on the size of the dog. Following the albuterol, use the nebulizer with 2–3 cc of sterile saline. Some pets have side effects from albuterol although that is rare. Sometimes side effects are seen, such as nervousness, a rapid heart rate or excessive panting, and they will disappear within an hour or so. If this happens, report it to your veterinarian for a possible adjustment of dosage or change in frequency of treatments.
If your veterinarian has not previously written a prescription for albuterol, for which there is no veterinary version, here is an example of how to write it.
Albuterol 0.083% 2.5 cc vials × 25
sig: using a nebulizer, administer q8–24hr as directed
Albuterol comes in a box of 25 vials, each containing 2.5 cc.
- Your veterinarian will prescribe the dose of albuterol for your pet.
- Nebulize the computed dose of albuterol; if it is 1 cc or less, mix it with 1 cc of saline solution.
- Nebulize an additional 2–3 cc. of saline after the albuterol treatment is completed.
Warning: Albuterol should not be administered to pets by people who have heart or lung disorders. Ask your physician if it is safe for you to be exposed to the albuterol mist given off during nebulization.
Saline decreases the thickness of mucus and helps moisturize the bronchioles, which helps the pet cough up debris blocking the lungs. Saline solution can be obtained from your veterinarian, or nebulizer saline can be obtained online.
Do not use saline solution intended for contact lenses.
Antibiotics such as gentocin or amikacin, which are intravenous antibiotics, can be mixed with saline. These drugs can be hard on the kidneys, so ideally it is best to monitor kidney function with blood and urine tests. These antibiotics are more kidney friendly when given with a nebulizer than when given intravenously.
Preventing Aspiration Pneumonia
Nebulizer treatments with either saline and/or albuterol can help prevent recurrence of aspiration pneumonia in pets with megaesophagus, pneumonia or bronchitis, and may be helpful in managing laryngeal paralysis by helping to clear aspirated debris from the lungs. Ask your veterinarian if your pet should have a preventive treatment daily, every other day or twice weekly.