Aural Hematoma in Dogs and Cats
Why is an Aural Hematoma a Problem?
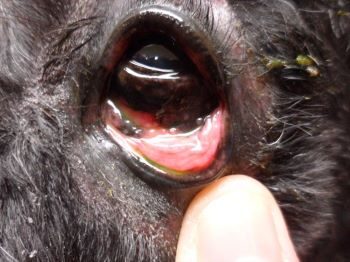
A hematoma is swelling created by a broken blood vessel after bleeding has occurred inside a tissue. Hematomas in the earflaps (aural hematomas) occur when head shaking breaks a blood vessel within the earflap. The earflap may partially or completely swell with blood. The swelling may be so large that the opening of the ear canal is occluded. The extra weight of the earflap may be uncomfortable and may lead to a permanent change in the carriage of the ears. This condition is more common in dogs but can occur in cats as well. The earflap will feel fluctuant and fluid-filled, like a water balloon.

A small hematoma may not actually be a problem and may not require repair. There are several situations where the hematoma should be repaired.
- The hematoma is so big that the ear canal is occluded (blocked). If this is the case, the ear cannot be evaluated for infection, nor can any infection be treated. In this situation, the hematoma must be relieved before the ear canal can be accessed.
- The hematoma is in a location where natural healing will create scarring in such a way that the ear canal will be permanently narrowed. A permanently narrow ear canal can predispose the patient to a lifetime of ear infections. This is particularly a problem in cats.
- The hematoma should be repaired if the owner feels the heavy ear flap is unacceptably uncomfortable for the pet.
- To maximize the ability of the ear flap to stand up straight after hematoma resolution or to prevent excessive scarring in the ear flap for cosmetic reasons.
What do we do to Relieve it?
There are probably as many ways of correcting ear hematomas as there are veterinarians. Some veterinarians have good results using medical therapy, treating with a corticosteroid. Some veterinarians will use surgery or low-level laser therapy in the treatment regimen for aural hematomas. You and your veterinarian need to discuss the best way to treat your pet. The following are some of the commonly performed procedures.
Aspiration
This procedure involves simply using a syringe to remove the fluid contents from the hematoma. The problem is that a space is left behind when the fluid is removed, and this space readily refills with more fluid leading to only temporary results. The benefits of the aspiration method are that it is inexpensive and relatively easy to perform, but the disadvantages are that it may introduce infection and may require multiple attempts. If the clot in the hematoma is already well organized and on its way to scarring, there may not be much fluid left to aspirate, and the technique may not work at all. Usually, other methods are utilized.
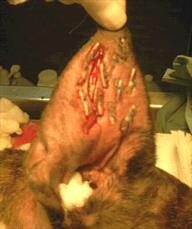
Pie-Crusting Sutures
Here, an incision is made in the earflap surgically. The hematoma is drained of fluid and blood clots. To prevent the hematoma from refilling with fluid, multiple sutures are placed in the hematoma area either vertically or horizontally, either partly or completely through the earflap, with or without ear cartilage removal. Sometimes bandages are applied post-operatively, sometimes not. Sutures are generally left in place for three weeks to allow good scarring to take place so that refilling will not occur. The earflap is essentially quilted to close any space where fluid might refill.

Teat Cannula Placement
A teat cannula is a small device used in the treatment of udder inflammation in cows. It can be placed in the opening of the teat to allow drainage of milk or infected discharges. Teat cannulas can also be surgically placed in a dog’s aural hematoma if the earflap is large enough to accommodate the device. The hematoma is drained of fluids and allowed to heal over the next several weeks. This method is generally successful but does involve the dog tolerating a gadget inserted in its earflap for several weeks as well as accompanying fluid drainage.

What if there is a Concurrent Ear Infection?Usually, there is a reason why a dog has been shaking his head: an ear infection. This means that the ear infection must be treated along with the hematoma. The ear will need cleaning, a microscopic examination of the discharge, and medication. Sometimes ear shaking just happens and there is no underlying infection, but be prepared for the expense and trouble of treating an ear infection along with that of the hematoma.
What if We Leave it Alone?
If left alone, an ear hematoma will resolve by itself. The fluid will be re-absorbed back into the body and the earflap will no longer bulge. The problem is that a lot of scarring is associated with this process and the ear is often not cosmetically appealing afterward (i.e. it becomes a “cauliflower” ear). Resolution of a large hematoma can take several months during which it may be uncomfortable for the pet. If the patient is a poor anesthetic risk, it is certainly reasonable to forgo surgery. Corticosteroids, such as prednisone, can be used to reduce scarring.
Aural Hematoma in Cats
The situation in cats is somewhat more complicated than in dogs largely because the cartilage in the feline ear is more sensitive to inflammation and scarring is more severe. This makes the untreated hematoma more likely to form a permanently narrowed ear canal and long-term ear infection potential. Cats’ ear cartilage tends to experience more healing deformity than dogs’ ear cartilage and more curling and softening of the thinner pinnal areas is seen.

What this comes down to is that there is less leeway in letting the ear heal on its own in cats than dogs. Surgical repair is especially important as there is a greater tendency for a cat’s canal to narrow. That said, a more natural cosmetic appearance of the actual ear flap is harder to achieve in cat than dogs. It is more important to focus on the function.
As with dogs, a cat’s hematoma is generally brought about by ear infections and subsequent head-shaking. (In cats, most ear infections stem from ear mites but there are plenty of exceptions.) Bandaging is often used post-operatively as is the Elizabethan collar to protect the ear from being scratched. The cat will need confinement during a healing period of approximately 3 weeks.